Should You Take Metformin for Prediabetes?
- By Hallie Levine
- Fact-checked by Joy Ferguson
- June 22, 2023
We get it: Those big guzzlers at the movies or Saturday morning donuts can be pretty tasty. But they can lead to blood sugar spikes and crashes that over time, predispose you to diabetes. If your doctor has mentioned prediabetes (and a medication called metformin), you’re also not alone. More than one in three Americans has prediabetes: a condition where blood sugar levels are higher than normal, but not high enough to be diagnosed as type 2 diabetes.
Prediabetes is a serious condition that raises your risk for developing type 2 diabetes—and also (unfortunately) to have a heart attack or stroke. More than 80 percent of people with this condition have no clue they have it, according to the Centers for Disease Control and Prevention (CDC).
The good news is there’s a lot you can do to help prevent prediabetes from progressing. Here’s what you need to know, and how metformin comes into play.
What is ‘Prediabetes,’ Exactly?
When you have prediabetes, your cells don’t respond normally to insulin.
Insulin is a hormone your pancreas makes that allows blood sugar into your cells to use as energy. And when your cells don’t respond to it normally, your pancreas makes more and more insulin to try to get your cells to react. When your pancreas can’t keep up, your blood sugar goes up—setting the stage for prediabetes.
Unfortunately, prediabetes doesn’t always cause symptoms, so you may not even know you have it. “The first step in treating prediabetes is getting diagnosed,” says Janet O’Mahony, M.D., an internal medicine specialist at Mercy Medical Center in Baltimore, Maryland.
It’s wise to talk to your doctor about diabetes screening if you have any of the following risk factors:
- You’re overweight or obese
- You’re 45 or older
- You have a parent, brother, or sister with type 2 diabetes
If you have some or all of these risk factors, you can get a simple blood sugar test to determine if you have prediabetes.
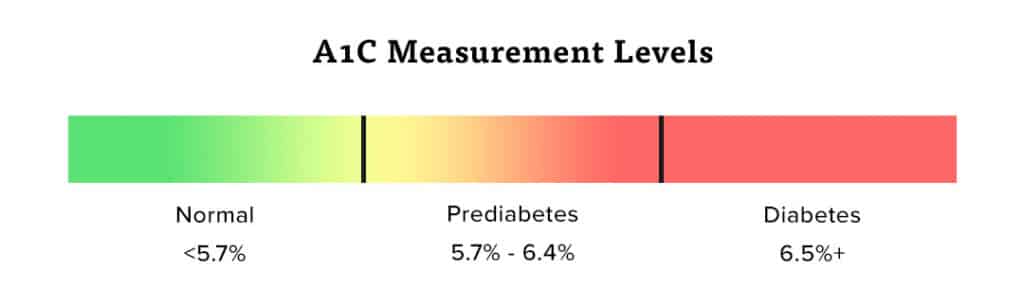
The best one is the A1C test, according to the American Diabetes Association. It measures your average blood sugar level over the past couple months. An A1C measurement below 5.7% is normal. Between 5.7 and 6.4% however, means you have prediabetes, and 6.5% or higher indicates diabetes.
If your A1C is between 5.7 and 6.4%, your chance of developing diabetes increases, to the tune of roughly ten percent per year, O’Mahony says. “You will want to make some changes to avoid developing full diabetes,” she notes.
How Does Metformin Work for Prediabetes?
It’s an oldy: Metformin and its use dates back centuries. According to a report published in the journal, Diabetologia, metformin is derived from the herb Galega officinalis, which was used to treat digestive ailments (1).
In 1918, scientists determined that one of the herb’s ingredients, guanidine, lowered blood sugar. It was rediscovered decades later—and modern metformin was used to treat diabetes in Europe in the 1950s. In 1994, metformin was FDA approved for use in the United States and today is the most widely prescribed glucose-lowering medication worldwide.
It’s pretty effective, too. In one study, researchers found metformin reduced the incidence of diabetes by 18% (2).
“It’s very effective, is inexpensive, and has very few side effects,” explains Gary Scheiner, MS, CDCES, owner of Integrated Diabetes Services in Wynnewood, Pennsylvania.
How Does Metformin Prevent Prediabetes?
“Metformin reduces how much glucose (sugar) is released from your liver, where it is commonly stored,” explains Scheiner. “And it delays or prevents the transition from prediabetes to diabetes.”
Metformin is particularly effective in preventing diabetes for the following groups, notes O’Mahony (3):
- People who are severely obese (an BMI of over 35)
- People under the age of 60
- Women with a history of gestational diabetes
Other Health Benefits of Metformin
Preventing full-blown diabetes isn’t the only benefit to taking metformin if you have prediabetes. The medication may also:
Lower cancer risk
A scientific review published in 2021 revealed that study participants with type 2 diabetes who had taken metformin had reduced their risk of developing cancer by about thirty percent (4).
Reduce risk of heart attack or stroke
In some studies, metformin has been shown to reduce the risk of heart disease and stroke. One theory is that it helps reduce levels of pro-inflammatory proteins in the body that are associated with heart disease, according to a study published in 2019 (5).
Lower risk of dementia
A review of 14 studies published in 2018 in the Journal of Alzheimer’s Disease found that in six studies, diabetic subjects taking metformin had reduced the incidence of dementia by about 24 percent (6).
How To Know if Metformin Is Right for You?
Talking to your doctor about metformin for prediabetes is a good first step.
There’s very little downside to taking it. Very rarely, metformin can cause a life-threatening condition called lactic acidosis (basically a build-up of too much lactic acid in the body). The risk for complications rises if you:
- Have kidney, heart, or liver disease
- Have ever had a heart attack, stroke, or diabetic ketoacidosis
- Drink regularly or binge drink
- Take certain other medications, such as methazolamide (for glaucoma), and anti-seizure drugs like topiramate (Topamax, in Qsymia), zonisamide (Zonegran), and others
“Metformin is a generic drug that is inexpensive,” O’Mahony notes. “It takes some getting used to because it can cause some nausea or diarrhea when you first start taking it.”
You may be able to avoid this by starting with a low dose, and building up gradually, she adds.
It’s best to talk with a healthcare professional (Hone can help with that!) before taking metformin for prediabetes to rule out any possible contraindications. And if you do experience adverse symptoms while taking the medication, stop immediately and call your doctor.
Other Ways To Treat Prediabetes
Metformin works well, but it’s still wise to approach your health from every angle (which can also include, perhaps sadly, fewer donuts). “The best strategy would likely be to combine metformin and lifestyle changes,” O’Mahony advises.
Some of the top tweaks you can make include:
Weight loss
According to the CDC, if you’re overweight, losing even five percent of your body weight can help reduce your risk of developing type 2 diabetes.
What’s more, a study published in 2019 also revealed that when those with type 2 diabetes lost at least ten percent of their body weight in the first five years after diagnosis—they were about twice as likely to go into remission than those who didn’t (7).
Exercise
Working out has been shown to help reverse prediabetes, and some research even suggests that more exercise—about five hours of activity a week—can be beneficial (8).
Spreading out your workout time helps, too. “Exercising at least six days a week can be even more beneficial than exercising for the ‘standard’ recommendation of 150 minutes per week,” Scheiner adds. “This is because the physiologic adjustments your body makes during and after activity make your cells more sensitive to insulin, yet the beneficial effects start to wane by the next day.”
Healthy eating
Following a Mediterranean-style eating pattern—rich in healthy fats, whole grains, beans, nuts, fruits, and vegetables, and low in processed meats, sugars, and refined carbohydrates—can help prevent or even reverse type 2 diabetes according to a review published in 2020 (9).
It can be tough to make these changes on your own, which is why O’Mahony recommends support and education programs. “These programs are called Diabetes Prevention Programs, and they are often paid for by your health insurance,” she explains.
In the meantime, talk to your doctor and see if taking metformin for prediabetes could be right for you.
Metformin may help you lose weight and ward off age-related illnesses.
References
1. Bailey, C. (2017). Metformin: Historical Overview
2. Diabetes Prevention Program Research Group. 2015. Long-term Effects of Lifestyle Intervention or Metformin on Diabetes Development and Microvascular Complications Over 15-Year Follow-Up: The Diabetes Prevention Program Outcomes Study
3. Moin, T. et al. (2018). Review of Metformin Use for Type 2 Diabetes Prevention
4. Zhang, K. et al. (2021). Metformin and Risk of Cancer Among Patients with Type 2 Diabetes Mellitus: A Systematic Review and Meta-Analysis
5. Han, Y. et al. (2019). Effect of Metformin on All-Cause and Cardiovascular Mortality in Patients with Coronary Artery Diseases: A Systematic Review and an Updated Meta-Analysis
6. Campbell, J. et al. (2018). Metformin Use Associated with Reduced Risk of Dementia in Patients with Diabetes: A Systematic Review and Meta-Analysis
7. Dambha-Miller, H., et al. (2019). Behavior Change, Weight Loss and Remission of Type 2 Diabetes: A Community-Based Prospective Cohort Study
8. Fritsche, A. et al. (2012). Different Effects of Lifestyle Intervention in High- and Low-Risk Prediabetes: Results of the Randomized Controlled Prediabetes Lifestyle Intervention Study (PLIS)
9. Martin-Pelaez, S. et al. (2020). Mediterranean Diet Effects on Type 2 Diabetes Prevention, disease Progression, and Related Mechanisms