Does Your Oxygen Level Drop When You Sleep?
Pulse oximeters used to be something you only saw at a doctor’s office or hospital to measure the saturation of oxygen in your red blood cells (they’re those gizmos that clamp onto your index finger and give off an E.T.-like red glow). But in the past few years they’ve become a staple on wearable trackers.
The Apple Watch, Garmin fēnix, and Oura Ring (among others) have added blood oxygen saturation level (also called peripheral capillary oxygen saturation or SpO2)—sensing to the long list of health metrics their smart wearables can track. These devices use infrared light to take repeated blood oxygen readings 24/7, assembling the data points into graphs that illuminate trends over time.
Why bother? As it turns out, your blood oxygen levels—especially during sleep—can serve as an early warning system, alerting you about potential or silent health problems like sleep apnea or chronic breathing issues that can cause you health problems now and shorten your healthspan.
Here we explore what SpO2 numbers mean, what normal oxygen levels are during sleep, and what to do if they dip.
Can you trust your smart device?
According to one study on the Apple watch, your wearable’s oxygen-sensing capabilities come close to rivalling the typical pulse oximeter that clips to your finger. (1).
“Sleep trackers’ pulse oximetry is generally accurate,” says Chris Winter, M.D., a sleep specialist who hosts the podcast Sleep Unplugged with Dr. Chris Winter. “It’s not difficult technology.”
There are, however, some situations that may throw off the reading, for example:
- Not strapping a smartwatch snugly to your wrist
- Moving while your device is attempting to take a reading
- Having your arms at your side or hands in a fist position
What Does Your Blood Oxygen (Sp02) Reading Actually Mean?
Sp02 tells you how saturated your blood is with oxygen. Most healthy people maintain blood oxygen levels of 95 percent or higher, on average. That said, it’s normal and healthy for readings to go up or down by several percentage points—both during the day and the night—based on activity, breathing rate, and body position.
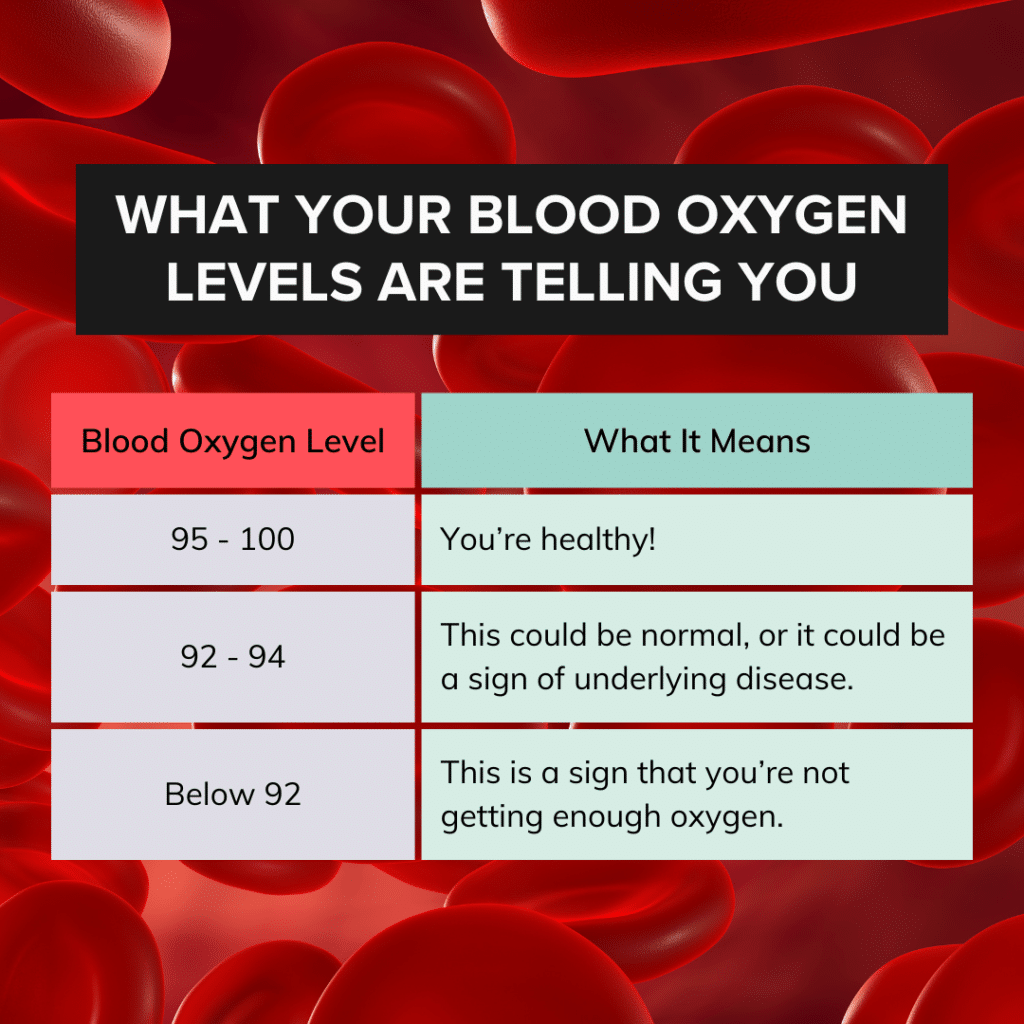
Periodic readings under 95—or even 92— aren’t necessarily a cause for concern.
First, one or two low readings could be a fluke. Body position, hand or wrist temperature, and movement can all affect your reading, says Winter.
Another factor: altitude. Let’s say you flew from the Jersey shore (sea level) to Crested Butte, Colorado (8900 feet above sea level). “Altitude can cause blood oxygen to drop below 95 for the few days it takes to become acclimatized,” says Winter (2).
“But nighttime readings that regularly dip below 93 are worth a conversation with your doctor,” he says.
With those caveats out of the way, let’s dive into three red-level situations—and what it might mean for your health if your oxygen levels dip below normal while you sleep.
Situation #1: Your normal average oxygen level during sleep is usually above 95+, but lately, it has trended downward.
A few things might be going on here.
If you had a nightcap, it can show up in your readings. In one study, participants who had a nightcap 30 minutes before bed, experienced aggravated sleep apnea symptoms (3).
“Alcohol before bed may cause breathing irregularities that can result in a decline in blood oxygen levels,” says Winter.
Another possibility: You have an upper respiratory infection. Like alcohol, a stuffy nose may make it more difficult for you to breathe at night. Pneumonia can also lower blood oxygen levels (4).
“If an infection causes your respiratory rate to rise above 23 breaths a minute, seek medical attention,” says Winter.
Situation #2: Your blood oxygen consistently remains below 92, day and night.
You may have a lung problem, such as asthma or chronic obstructive lung disease, says Winter. This is definitely something to mention to your doctor.
Situation #3: Your blood oxygen levels repeatedly go up and down while you sleep.
If your device records some night-time readings below 92 and others above 95, it may be a red flag for sleep apnea, which some sources estimate affects about 34 percent of middle-aged men (5).
People with sleep apnea stop breathing for 10 seconds or longer, five, 15, 25, or more times per hour. Their brains sense the dropping oxygen levels and repeatedly wake them to breathe. Still, by morning, many people with sleep apnea don’t remember their restless night. That’s why oxygen trackers are so helpful, says Winter.
Sleep apnea is especially likely if—in addition to low Sp02 readings—you’re also excessively tired during the day, your partner won’t stop complaining about your snoring, or you wake with a headache, says Winter.
If you think you might have the condition, mention it to your doctor.
“In addition to raising your risk for many deadly diseases, sleep apnea may also speed up aging throughout your body,” says Winter.
What Makes Sleep Apnea so Dangerous?
To help people understand why sleep apnea is so deadly, Winter likes to use the analogy of two people who set out to explore a submerged shipwreck. One person is equipped with a scuba tank, the other with snorkeling gear.
The scuba diver can swim down and explore for a half hour or so. The snorkeler, however, must resurface roughly every 45 seconds to gulp down more air.
“This is what it’s like for someone with sleep apnea,” he says.
People with sleep apnea wake repeatedly, which reduces how much time they spend in deep, restorative sleep. (6)
“This sleep fragmentation can reduce the brain’s ability to flush toxins during sleep, increasing the risk for memory problems,” says Winter. “On top of that, when you stop breathing for 10 seconds or longer, pressure builds up in your chest, raising your risk for heart problems. Finally, cells throughout your body are intermittently deprived of oxygen.”
All of this creates a toxic brew, upping your risk for just about everything that can cut your life short (8).
“Sleep apnea can raise your risk for many life-threatening diseases and situations, such as atrial fibrillation, high blood pressure, chronic inflammation, stroke, diabetes, hardening of the arteries, and even car accidents through tiredness,” says Winter.
Sleep apnea has also been linked to low testosterone levels, erectile dysfunction, and low libido.
On top of all that, sleep apnea speeds up aging in three key ways.
Faster cellular aging
In a study of 622 adults, for each standard deviation increase in the apnea-hypopnea index (a diagnostic tool for determining the presence and severity of sleep apnea), people’s cells aged roughly 215 days (8).
Accelerated telomere shortening
The protective caps on the ends of chromosomes, telomeres are heavily involved in cell division. Whenever cells divide, telomeres shorten. Once telomeres get too short, cells can’t divide at all. Nobody gets through life without some telomere shortening. (9) “Sleep apnea seems to accelerate the process,” says Winter.
Less robust mitochondria
The power factories of cells, mitochondria can lose their effectiveness with age, starving cells of energy and creating byproducts that harm tissues. One study found that in subjects under 50 years of age, sleep apnea was associated with an increase in specific hallmarks of aging, such as dysfunctional mitochondria (10).
Do You Need a CPAP to Treat Sleep Apnea?
You might. Though many other treatments exist—from dental devices to surgery—CPAP machines remain the gold standard for treating sleep apnea.
Short for “continuous positive airway pressure,” CPAPs blow air into your nose and/or mouth to keep your airways open while you sleep. They may help you reverse some of the accelerated aging mentioned above, research suggests (11, 12).
That said, not everyone with sleep apnea needs a CPAP, says Winter, who compares mild sleep apnea (defined as fewer than 15 apneas per hour) to someone who smokes one cigarette a month.
“It would obviously be better if they didn’t smoke at all,” he says, “but someone who smokes four packs a day has a much higher risk of disease than someone who has one cigarette a month.”
It’s similar to sleep apnea, he says. In fact, if you only stop breathing fewer than five times per hour, sleep specialists sort you into the “normal category.” One exception: If you feel like hell and are falling asleep while driving, a CPAP machine could be life-changing, regardless of how many apneas you experience per hour, Winter says.
References
1. L. Zumerkorn Pipek (2021): Comparison of Sp02 and Heart Rate Values on Apple Watch and Conventional Commercial Oximeters Devices in Patients with Lung Disease.
2. Rojas-Camayo, J., et al. (2018). Reference values for oxygen saturation from sea level to the highest human habitation in the Andes in acclimatized persons.
3. Izumi, I., et al. (2005). Effect of moderate alcohol intake on nocturnal sleep respiratory parameters in healthy middle-aged men.
4. Chatterjee, N. A., et al. (2021). Admission respiratory status predicts mortality in COVID-19.
5. Yeghiazarians, Y., et al. (2021). Obstructive Sleep Apnea and Cardiovascular Disease: A Scientific Statement From the American Heart Association.
6. Roy, B., et al. (2022). Impaired Glymphatic System Actions in Obstructive Sleep Apnea Adults.
7. Diamond, J. A., & Ismail, H. (2021). Obstructive Sleep Apnea and Cardiovascular Disease.
8. Li, X., et al (2019). Association between sleep-disordered breathing and epigenetic age acceleration: Evidence from the Multi-Ethnic Study of Atherosclerosis.
9. Carroll, J. E.,et al. (2019). Obstructive sleep apnea, nighttime arousals, and leukocyte telomere length: the Multi-Ethnic Study of Atherosclerosis.
10. Pinilla, L., et al. (2021). Association of Obstructive Sleep Apnea with the Aging Process.
11. Cortese, R., et al. (2022). Epigenetic age acceleration in obstructive sleep apnoea is reversible with adherent treatment.
12. R. Cortese et al (2022) DNA Methylation Clocks Reveal Epigenetic Age Acceleration in Obstructive Sleep Apnea Which is Reversible with Adherent Treatment